If you’ve ever donated blood or had a blood transfusion, you’ve probably read a blood bag label. Blood bags and blood bag labels play an important role in medical care. We need blood to survive and carry oxygen to different parts of the body. With or without a pandemic, the body needs blood to fight off infections, viruses and bacteria. Blood transfers play a key role in patient health.
Patients may require a blood transfusion for a myriad of different reasons. These can include surgeries, injuries with significant blood loss, bleeding disorders or diseases. In all of these cases, patients receive donor blood. Depending on the condition, a patient may need red blood cells, white blood cells, plasma or platelets. But more importantly, the donor’s blood type must be compatible with the recipient.
Blood bag labels can help medical professionals determine which blood bag to use for each patient. These distinctions prevent fatalities and further complications that could arise from a mismatched blood donor. Effective, safe and sterile blood bag labeling belongs in any blood transfusion process.
What Do You Use Blood Bags For?
Blood bags are bags that contain blood, whether it’s whole blood or a part of the blood needed for the patient’s purposes. Typically, blood bags should be disposable and sterile. They are often made of a specific kind of plastic; poly vinyl chloride. Medical professionals can use blood bags to collect, store, process and distribute blood when necessary.

The blood bag consists of several small parts that all serve important functions. These include the bag itself, the donor tube, transfer bags and a clamp. The donor tube comes with a needle to draw the blood.
Blood bags come in different forms for different uses. A single bag will contain the whole of the blood, without separating it into parts. A double bag will separate the packed cells from the plasma. A triple bag separates the packed cells, plasma and platelets. Finally, a quadruple bag will separate the packed cells, platelets, plasma, and cryoprecipitate.
Cryoprecipitate comes from plasma. Providers create it by by freezing and then centrifuging plasma. The cryoprecipitate helps blood clot properly with its high density of proteins. For people with rare blood disorders like hemophilia and von Willebrand disease, clotting is difficult because of a lack of proteins. Cryoprecipitate can help patients with these conditions slow bleeding or stop it altogether.
Before a transfusion or collecting blood from a donor, medical professionals test the patient or donor to see what type of blood they carry. Matching the donor’s blood type to the patient’s can spell the difference between life and death. Blood comes in four types: A, B, AB, and O. It is measured by whether or not it is Rh positive or Rh negative. Donors are also screened before they donate blood to determine whether or not they have contagious, blood-borne diseases, like hepatitis or HIV.
Medical professionals need to be able to mark the difference between bags of blood in order to avoid fatal reactions to the wrong blood transfusion.
How are Blood Bags Labeled for Use and Storage?
Blood bag labels play a crucial role in the health of a patient. If a patient receives the wrong blood type, they can have worsening symptoms, or a fatal reaction. Should the patient have O-type blood and receive any other kind of blood type, they can develop a major hemolytic transfusion reaction.
During these reactions, the patient’s immune system draws the transfused blood towards it. Cells rip apart and organs release bad chemicals into the body. Kidneys begin to fail. Patients begin to develop an illness with symptoms that feel like the flu. They can go into shock and eventually die.
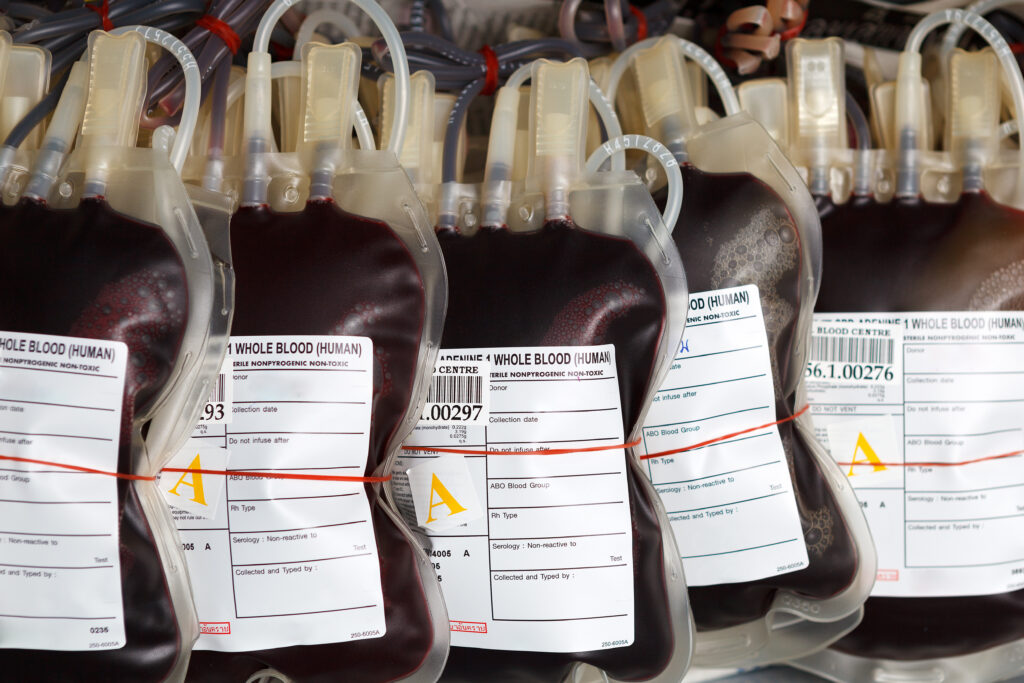
The life of a patient who requires a blood transfusion depends upon the ability to determine the difference between blood bags in storage. These labels must be able to withstand freezing cold and incredibly hot temperatures, while maintaining the integrity of the writing on the blood label. According to blood bag label standards, there are two reasons labels should also be waterproof. First, the bag may be sterilized. Secondly, a patient could receive a transfusion in a warm bath or near a body of water. Blood itself has many liquid components, which adds to the need for a waterproof label.
Never pack bags tightly. Place the label on each bag so that it does not come off at any time. If you are storing platelets alone, make sure you agitate them constantly to maintain their integrity in storage. A blood label must withstand up to five days of constant movement to allow the bag to be properly identified.
Blood labels should also conform to the shape of the bag. Since blood bags don’t have a particular shape when they are full, the blood bank label should be able to shift with the bag as needed. Otherwise, it might fall off in the process.
What Kind of Information Is Needed on the Label?
Two types of blood product labels exist for blood bags: primary labels and secondary labels. Bag manufacturers apply primary labels during production. These labels contain the manufacturer’s name and address, as well as reference numbers, batch numbers, and codes. These identifying markers help both the manufacturer and the medical facility trace the whereabouts of the bag.
Secondary blood type labels contain crucial pieces of information for donors and patients. It’s important to display the donor’s identification number, the collection date and the blood type in prominent type. This helps medical professionals distinguish the different types of blood. It is also important to be able to see the expiration date so that patients do not receive expired blood. Furthermore, the secondary blood label features a product code and the matrix tracking barcode.
Tracking blood bags with blood type labels can also spell life or death for patients. Sometimes, this screening detects an unknown contagious or bloodborne illness the donor was unaware of. If the screening detects something after donation it is important to track down and dispose of the contaminated bags. Afer collecting donations, human error can lead to the mislabeling of a donor’s blood type. Should this instance occur, medical professionals and staff need to be able to track down the mislabeled bags in order to prevent fatal reactions to the wrong types of blood.
Related: Is your blood bag labeling compliant?
What Kind of Conditions are Blood Bags/Labels Put Under?
Blood bags and the blood type labels endure many kinds of conditions. Depending on the nature of the blood or components needed, providers may freeze the bag, place it in room temperature storage, sterilize it with hot water, or subject it to steam from a patient’s warm bath. While the plastic bags can usually take this kind of beating, it is important to use the right kind of blood bag labels to preserve the identifying information on the bag.
Before reaching a patient, donor staff handle the blood bag and its respective blood bank labels first. After they fill five tubes or so with blood, they fill the bag itself with more blood. They also fill the bag with an anticoagulant. Typically, the anticoagulant consists of Citrate Phosphate Dextrose Adenine, or CPDA. Citrate chelates calcium, preventing the donated blood from coagulating, or growing hard. Dextrose maintains the metabolism found in the red blood cells. Phosphate lowers acidity. Adenine makes red blood cells more viable for the recipient of the donated blood.
Staff seals off excess tubing and discards it. Then they tie the bags and tubes up in an elastic band and place them in coolers. The blood bank labels must survive all of these actions. Next, they attach smaller plastic bags to the main bag, along with a bag full of nutrient fluid. Then the components tech attaches secondary blood bag stickers, indicating the plasma requirement. After that, the tech pours the entire bag of blood into a centrifuge cup and spins it, like a washing machine, to separate the components. Plasma rises to the top. The tech collects it and places in a secondary bag attached to the main bag
After collecting the plasma, the tech removes all the extra liquid and stores it in separate bags. The main bag is now the RBC (red blood cell) bag. This bag is then mixed and hung on a pole that looks like a shower hook. White blood cells are removed and placed in a container that looks like a compact. The RBC bag is then stored in a cooler at 39 degrees Fahrenheit.
You must freeze the bags to properly store plasma. These bags must be at -4 degrees Fahrenheit.
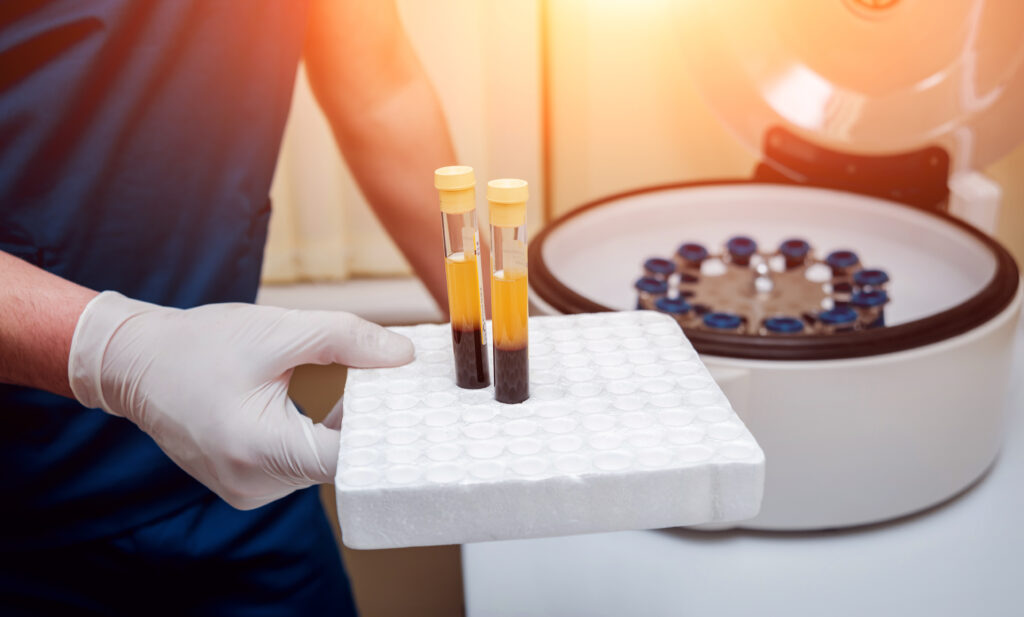
Meanwhile, staff test the blood in the five test tubes. This helps identify any viral or bacterial infections that the donor may not have known about. Medical staff receive these results and make sure the blood bag stickers reflect the results. If blood bags are fit for transfer, they go to hospitals and other medical facilities for patient use.
What Kind of Materials Should These Blood Bag Labels Have?
Blood bag labels should be water and temperature resistant in order to survive the cycle from the donor to the recipient. Some of these blood bag stickers have proved to be resistant to water. Their elements are composed of latex imbued paper, coated with clay. These two ingredients create a strong label that resists water from ice or baths. With this flexibilioty, providers can sterilize or freeze these labels. Printability is fair.
Other forms of labels have a white film facestock that breathes, so it does not absorb moisture from the outside elements. They can resist high temperatures, maintain stability, and conform to the shape of the bag. All of these qualities are crucial to the integrity of the label.
Furthermore, the secondary labels should be able to receive thermal transfer ribbons. White polyolefin thermal transfer printable film specially engineered to do so. A three-ply polypropylene film allows the labels to have identifying codes and names printed on them.
Adhesives should have a low migration level. They should stick to their original location, so that the bag does not lose the identifying labels. Furthermore, the adhesive should follow FDA standards so that it does not eat through the plastic and contaminate the blood specimens in the bag.
Are the Use of These Materials Regulated in Any Way?
The ISO has several blood bag label standards about the composition of a container and a label meant to carry and distinguish human blood samples. Some of these regulations apply to blood bag labeling and the adhesive on the blood product label. The FDA also regulates the kind of adhesive used for blood bags, along with the ISEGA.
Make sure you test these blood bag labels for safety before putting them into use. An adhesive that eats away at the plastic bag could be catastrophic. A label that falls off, or allows the ink on the label to wash away could lead to a recipient getting the wrong kind of blood any potentially dying. When it comes to patient health and well-being, even the tiniest details present the most importance.
Maegan Wagner, BSN RN CCM has over 10 years of healthcare experience. Her nursing career has led her through many different specialties, but her passion lies in educating through writing for other healthcare professionals and the general public.



